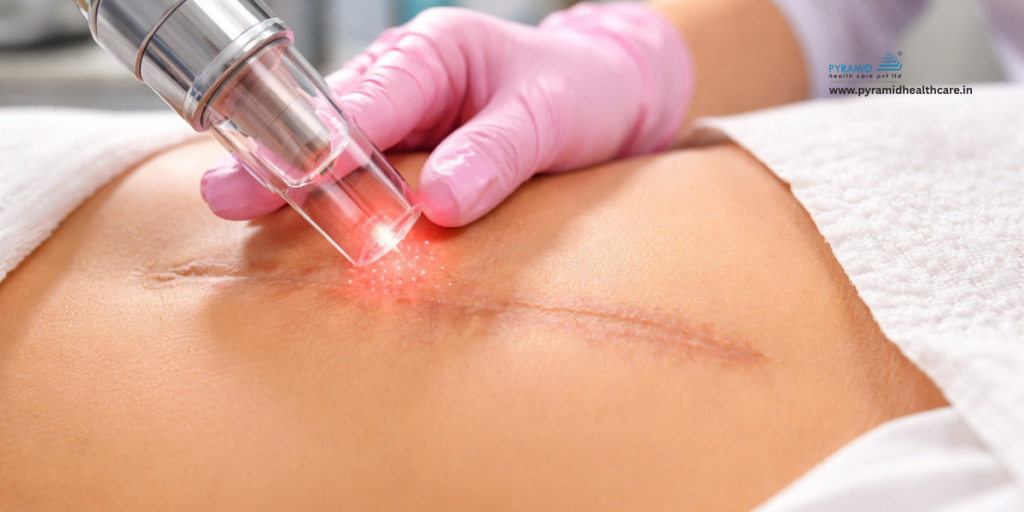
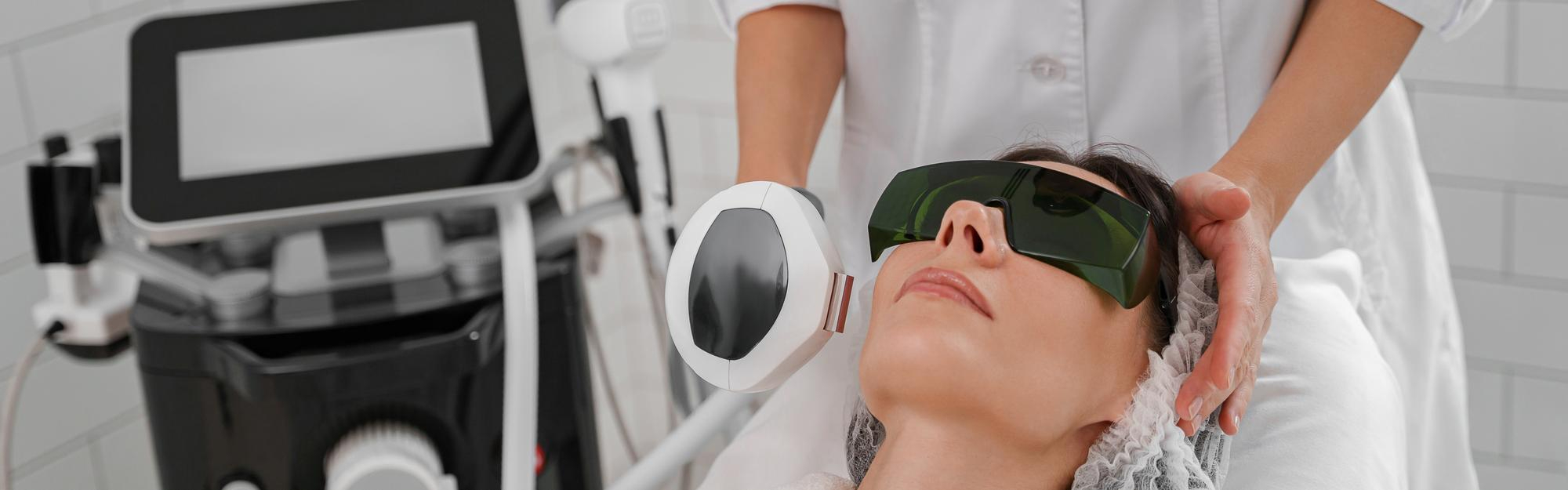
CO2 Laser for Surgical Scars: What Actually Works in 2026 (And What’s Just Hype)
By [Pyramid Healthcare] | Aesthetic Laser | Updated 2026
You survived the surgery. You healed. And then you looked in the mirror.
The scar is still there — raised, discolored, or sunken into the skin like a permanent reminder of something you’d rather put behind you. You’ve tried silicone sheets, vitamin E oil, and every “miracle” cream the internet has recommended. Some helped a little. None of them transformed it.
So now you’re here, researching CO2 laser treatment. You’ve heard it’s the gold standard. You want to know if it’s real — or if it’s just the next overhyped solution on a very long list.
This article gives you the clinical truth. No fluff. No fear-mongering. Just what the evidence shows, what the procedure actually involves, and whether you’re a good candidate for it in 2026.
What Is a Surgical Scar, Really?
Before discussing treatment, it’s worth understanding what you’re treating — because not all scars are the same, and CO2 laser (CO2 laser for surgical scars) works differently depending on scar type.
A surgical scar forms when the dermis (the deep layer of skin) is disrupted. The body responds by producing collagen to repair the wound. In an ideal healing environment, this collagen lies down in an organized fashion, and the scar fades over 12–24 months. In reality, numerous factors interfere: infection, tension on the wound edges, genetic predisposition, wound care compliance, and the location of the incision.
The result can be one of several scar types:
- Flat, hyperpigmented scars — The most common. Pink, red, or brown in color; roughly the same level as the surrounding skin.
- Atrophic scars — Sunken or depressed below the skin surface; common after procedures in areas with thin skin.
- Hypertrophic scars — Raised, red, and firm; remain within the boundary of the original incision.
- Keloid scars — Raised and extend beyond the incision boundary; caused by overproduction of collagen and have a genetic component.
CO2 laser is highly effective for the first three types. Keloids require a more nuanced approach — more on that later.
How the CO2 Laser Actually Works
CO2 (carbon dioxide) laser operates at a wavelength of 10,600 nm, which is selectively absorbed by water in the skin cells. When the laser energy is delivered to scar tissue, it vaporizes the outer layers of damaged skin and delivers controlled thermal energy into the deeper dermis.
This triggers two simultaneous healing processes:
- Ablation — The damaged surface cells are removed, eliminating discoloration and irregular texture at the epidermal level.
- Neocollagenesis — The thermal injury to the dermis stimulates fibroblasts to produce new, organized collagen and elastin. Over the following weeks and months, this new collagen gradually remodels the scar from within.
The result is skin that is smoother, flatter, better pigmented, and structurally rebuilt — not just resurfaced.
Fractional vs. Fully Ablative CO2
In 2026, the majority of surgical scar treatments use a fractional CO2 laser rather than the older fully ablative approach. Understanding the difference matters:
Fully Ablative CO2 removes the entire surface of the treated area. Results can be dramatic, but downtime is significant (10–14 days), and the risk of prolonged redness, infection, and post-inflammatory hyperpigmentation is higher. It remains appropriate for very deep or extensive scarring in certain patient populations.
Fractional CO2 (such as the Lumenis UltraPulse, Sciton Halo, or Solta Fraxel CO2) delivers the laser in thousands of microscopic columns, treating only a fraction of the skin at a time and leaving surrounding tissue intact. This dramatically accelerates healing, reduces downtime to 5–7 days, and lowers complication risk — while still delivering clinically significant collagen remodeling.
For most surgical scar patients today, fractional CO2 is the treatment of choice.
What the Evidence Says in 2026
This isn’t experimental. CO2 laser resurfacing for scars is among the most studied procedures in aesthetic dermatology and plastic surgery. Here’s what the clinical literature consistently shows:
- Improvement rates of 50–80% in scar appearance are commonly reported across studies for hypertrophic and atrophic surgical scars after a series of fractional CO2 treatments.
- Studies published in the Journal of the American Academy of Dermatology and Lasers in Surgery and Medicine have demonstrated significant improvements in scar height, texture, pigmentation, and pliability following CO2 laser therapy.
- A 2024 systematic review found that fractional CO2 laser, when used on mature surgical scars, produced statistically significant improvements in both objective (Vancouver Scar Scale) and subjective (patient-reported) outcomes.
- Combination protocols — pairing CO2 laser with PRP (platelet-rich plasma) or fractional radiofrequency — are showing enhanced results in 2026, particularly for deeper, more fibrotic scars.
It is important to be precise: a CO2 laser does not erase scars. It significantly improves them. Managing expectations with clinical honesty is not a weakness — it is the foundation of patient trust.
Who Is a Good Candidate?
Candidacy for CO2 laser on surgical scars depends on several factors. A thorough consultation with a board-certified dermatologist or plastic surgeon should always precede treatment.
You ARE likely a good candidate if:
- Your surgical scar is mature — at least 6–12 months post-surgery. Treating an immature scar with laser can worsen inflammation and delay normal healing.
- You have a hypertrophic, atrophic, or flat hyperpigmented scar.
- Your skin is well-hydrated and in good general health.
- You are not currently on isotretinoin (Accutane) — treatment should be deferred for at least 6 months after completing a course due to impaired wound healing.
- You have realistic expectations and understand that improvement — not perfection — is the goal.
- You are Fitzpatrick Skin Types I–IV. CO2 laser can be performed safely on darker skin types (V–VI) but requires more conservative settings, careful technique, and an experienced provider to minimize post-inflammatory hyperpigmentation risk.
You are NOT a good candidate if:
- Your scar is an active keloid. Laser on a keloid can provoke further aggressive growth. Keloids require intralesional corticosteroid injections, silicone therapy, or a multimodal approach — not CO2 ablation as a standalone.
- You have an active infection or inflammation at or near the scar site.
- You have a history of HSV (herpes simplex virus) and are not pre-treated with antiviral prophylaxis. CO2 laser can trigger a herpes outbreak in susceptible individuals — antiviral coverage is standard of care.
- You are pregnant or breastfeeding.
- You have unrealistic expectations or are seeking a procedure to achieve scar elimination rather than significant improvement.
The Treatment Process: What to Expect
Pre-Treatment (2–4 Weeks Before)
A well-prepared skin is a better-healing skin. Your provider may recommend:
- Topical retinoids to prime skin cell turnover (stopped 5–7 days before treatment).
- Tyrosinase inhibitors (hydroquinone, kojic acid, or azelaic acid) for darker skin types to reduce post-inflammatory hyperpigmentation risk.
- Antiviral medication starting 1–2 days before treatment for HSV-susceptible patients.
- Sun avoidance — sun-damaged or recently tanned skin increases complications.
- Photographs — a good clinic documents baseline appearance for comparison.
The Day of Treatment
The procedure is typically performed in the office. For small or isolated surgical scars, it may take 15–30 minutes. For larger areas, allow 45–90 minutes.
- Topical anesthetic cream is applied 45–60 minutes prior.
- For deeper treatments or anxious patients, oral sedation or local anesthesia may be offered.
- The laser handpiece is passed over the scar in precise, controlled passes. You will feel warmth and a sensation similar to a rubber band snapping against the skin — well-tolerated by most patients.
- Immediately after, the treated area appears red, swollen, and raw. This is expected and normal.
Post-Treatment Recovery (The Part No One Talks About Enough)
Recovery is where outcomes are won or lost. Patients who follow aftercare protocols meticulously heal faster and achieve superior results.
Days 1–3: Significant swelling, redness, and a weeping or “raw” appearance. Keep the area clean, apply prescribed healing ointment (petrolatum-based, such as Aquaphor), and avoid all sun exposure.
Days 4–7: Skin begins to form new surface cells. Peeling and flaking occur. Do not pick or forcibly exfoliate. The temptation is real — resist it entirely.
Week 2: Most patients are socially presentable, though persistent pinkness is normal and expected.
Weeks 3–12: The pink fades, new collagen continues to remodel, and the scar gradually improves. The full benefit of a single session may not be apparent for 3–6 months.
Sun protection is non-negotiable. SPF 50+ daily, for a minimum of 3 months post-treatment. UV exposure on newly resurfaced skin will cause hyperpigmentation that can be more difficult to treat than the original scar.
How Many Sessions Will You Need?
There is no universal answer — but here are honest clinical benchmarks:
- Minor, flat, hyperpigmented scars: 1–2 sessions, spaced 6–8 weeks apart.
- Moderate hypertrophic or atrophic surgical scars: 2–4 sessions, spaced 8–12 weeks apart.
- Deep or wide fibrotic scars: 4–6 sessions; may benefit from combination therapy (CO2 + PRP or microneedling RF).
Each session builds on the last. Collagen remodeling is a biological process — it cannot be accelerated beyond the body’s capacity. Patience is a clinical requirement, not a personal virtue.
CO2 Laser in 2026: What’s New?
The technology and protocols have meaningfully advanced. Here is what distinguishes current practice from treatment even five years ago:
1. AI-Assisted Treatment Planning
Several leading platforms now integrate AI skin analysis to guide laser settings based on scar morphology, depth, and skin type — reducing operator variability and optimizing energy delivery for individual patients.
2. Combination Protocols
A standalone CO2 laser is still effective. But combination approaches are producing superior results:
- CO2 + PRP (Platelet-Rich Plasma): PRP applied immediately post-laser accelerates healing and enhances collagen production. Multiple trials support improved outcomes with this combination.
- CO2 + Subcision: For tethered or depressed surgical scars, subcision (a minor in-office procedure that releases fibrous bands beneath the scar) followed by CO2 resurfacing addresses both the structural tethering and the surface texture simultaneously.
- CO2 + Microneedling RF: Alternating sessions of fractional CO2 and radiofrequency microneedling allow for deeper dermal remodeling with less cumulative surface trauma.
3. Exosome Adjuncts
Topical exosome serums applied post-CO2 treatment are gaining traction in 2026 as an accelerant to healing and collagen synthesis. Early clinical data are promising, though long-term large-scale studies are still emerging.
4. Improved Protocols for Skin of Color
The historical undertreatment of darker skin types with ablative lasers is being addressed. Conservative fractionation ratios, longer pulse durations, and the adjunctive use of pigment-suppressants pre- and post-treatment have made CO2 laser significantly safer and more accessible for Fitzpatrick V–VI patients when performed by experienced providers.
Risks and Honest Limitations
Every reputable provider has an obligation to present risk alongside benefit. For CO2 laser on surgical scars, the clinically documented risks include:
- Post-inflammatory hyperpigmentation (PIH): More common in darker skin types; usually manageable with topical agents.
- Prolonged erythema (redness): Typically resolves by 3 months; occasionally persists longer in sensitive or reactive skin.
- Infection: Risk is low with proper wound care; bacterial and herpetic infections are the most common.
- Scarring: Paradoxical worsening of scarring is rare but possible, particularly with overly aggressive settings or poor patient selection.
- Hypopigmentation: Loss of pigment in the treated area; more common with overly aggressive, fully ablative approaches.
These risks are minimized — not eliminated — by choosing an experienced, board-certified provider, following pre- and post-treatment protocols, and undergoing treatment at the right time in scar maturation.
The Right Provider Makes All the Difference
CO2 laser equipment is a tool. Its outcome depends almost entirely on the clinical judgment and technical skill of the person operating it.
When selecting a provider, ask specifically:
- Are you board-certified in dermatology or plastic surgery?
- How many CO2 laser scar treatments have you performed? Request before/after photographs of actual patients — not stock images.
- What laser platform do you use? Know the device.
- What is your protocol for darker skin types? (If you have Fitzpatrick IV–VI skin, this question is essential.)
- What is included in aftercare? A clinic that sells you a laser session and sends you home with nothing is not the right clinic.
Price should never be the primary driver of this decision. The cost of a complication — in time, money, and emotional toll — exceeds the savings of choosing the cheapest provider.
Is CO2 Laser Worth It for Surgical Scars in 2026?
Yes — with clear eyes and honest expectations.
CO2 laser is not a cosmetic trend. It is a medically validated, evidence-supported intervention that can meaningfully improve the appearance of surgical scars. For the right patient, treated at the right time, by the right provider, the results are clinically significant and life-quality-enhancing.
It is not a magic eraser. Scars treated with CO2 laser are improved scars — smoother, flatter, better integrated with surrounding skin, and significantly less visible. For most patients, that is a profound and lasting improvement.
If you have been living with a surgical scar and waiting for a sign to seek proper treatment, the evidence in 2026 is clear: CO2 laser works. The question is not whether to pursue it — it’s finding the right specialist to guide you through it.
Book a Consultation
If you’d like to explore whether CO2 laser treatment is appropriate for your surgical scar, Pyramid Healthcare offers comprehensive scar assessment consultations with our board-certified team. We evaluate scar type, skin type, treatment history, and candidacy before recommending any protocol.
Disclaimer: This article is intended for informational purposes only and does not constitute medical advice. Individual results vary. Consult a qualified medical professional before pursuing any laser treatment.
 Skip to content
Skip to content